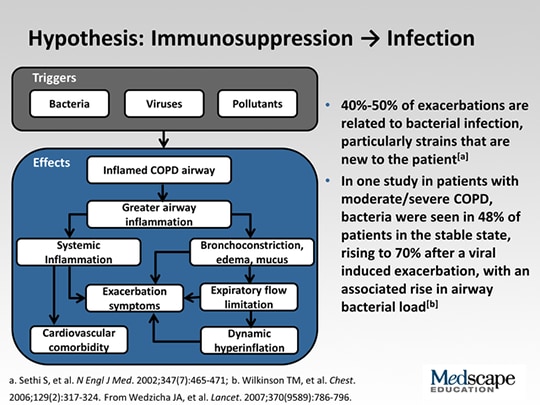
Results: Regarding the value of FEV 1 at the baseline, that in the LAMA/LABA group was 79.2% ± 6.4% and that in the Control group was 80.9% ± 6.4%, but that in the COPD groups was 57.9% ± 8.7% there was a significant difference between the COPD and the Control group (p < 0.0001). The patient-reported outcomes of the quality of life (PRO-QOL) were evaluated by the Cancer Dyspnea Scale (CDS), the COPD assessment test, and the St. The actual values were measured during the perioperative pulmonary function at three points of the preoperative baseline, the postoperative 1 week and the postoperative 4 weeks these changes and changed ratios were then calculated. The Control group had no treatment of the dual bronchodilator. The LAMA/LABA and the COPD groups daily received inhaled LAMA (50 μg) and LABA (110 μg) for 1 week before surgery and for least 4 weeks after surgery. Thirty-seven patients were enrolled as non-obstructive patients (70% ≤ %FEV 1), who were randomized into two groups, the LAMA/LABA (n = 19) and the Control group (n = 18). 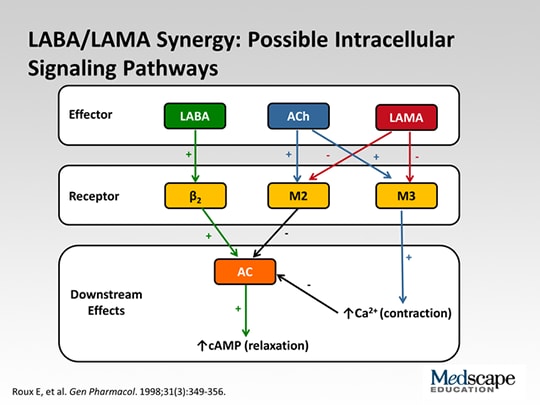
Methods: Based on the results of the preoperative pulmonary function test, 25 patients were diagnosed with COPD. To evaluate the effectiveness of the perioperative intervention of LAMA/LABA, a randomized prospective trial was performed for the lung cancer patients receiving a lobectomy with normal pulmonary function and COPD. Background: A dual bronchodilator, long-acting anticholine drugs (glycopyrronium, LAMA) and the long running β- 2 stimulant (indacaterol, LABA), are effective for the treatment of chronic obstructive pulmonary disease (COPD).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
